Where is the Vagus Nerve?
Vagus Nerve Anatomy-Where is the Vagus Nerve?
Nerves play a very important role in our body. Nerves form the basis of message conduction in the body. Some take messages from the brain to the body via spinal cord and some nerve fibers are responsible for conducting messages from the body parts like organs to the brain. Hence nerves form the basis of the nervous system which works efficiently by the collaboration of brain, spinal cord and nerves.
There are two types of nerves. Cranial nerves and spinal nerves. Furthermore, there are twelve cranial nerves. Each cranial nerve has its own definitive function. If any nerve fails to perform its own function, the entire system fails. The cranial nerves are olfactory nerve(CN I), Optic nerve(CN II), oculomotor (CN III), trochlear (CN IV), trigeminal (CN V), abducent (or abducens; CN VI), facial (CN VII), vestibulocochlear (CN VIII), glossopharyngeal (CN IX), vagus (CN X), accessory (CN XI) and hypoglossal (CN XII).
The nerve which will be discussed is Cranial nerve X which is named as Vagus nerve. Vagus nerve plays a vital role in the nervous system. It is the longest and one of the most complex nerves. To understand the anatomy of the vagus nerve, it is necessary to have conceptual clarity of its nuclei, the course it takes within the body and how to mark it over the body.
The first thing is how to locate it over the body, marking it on the surface of the skin. For that the first thing is to figure out the location of the Internal Jugular Vein. Then it is marked by two points. The first point is the tragus of the ear. The second point is the medial end of the clavicle. This is the surface marking procedure of the vagus nerve wne you want to locate it in the head and neck region.
Every cranial nerve has nuclei associated with it. These nuclei are basically aggregates of cell bodies of neurons and then the cranial nerves which are actually bundles of axons are attached to them. These nuclei can be either sensory or motor. They can never be both. The sensory nuclei deal with different sensations like touch, light sensations, sound, pain etc. The stimuli such as pain triggers a signal which is received by a nerve which takes it to the sensory nucleus and that nucleus sends the signal to the brain via more nerves.
The second kind of nucleus is the motor. Motor nuclei deal with the actions like moving of hands, moving hand away from a hot object etc.
Some nerves in our body are mixed, some our only sensory while others are just motor. Vagus nerve is a mixed nerve. Now the vagus nerve has 3 nuclei which are, main motor nucleus, Parasympathetic nucleus and sensory nucleus. The figure below explains the nuclear connections of the vagus nerve clearly.
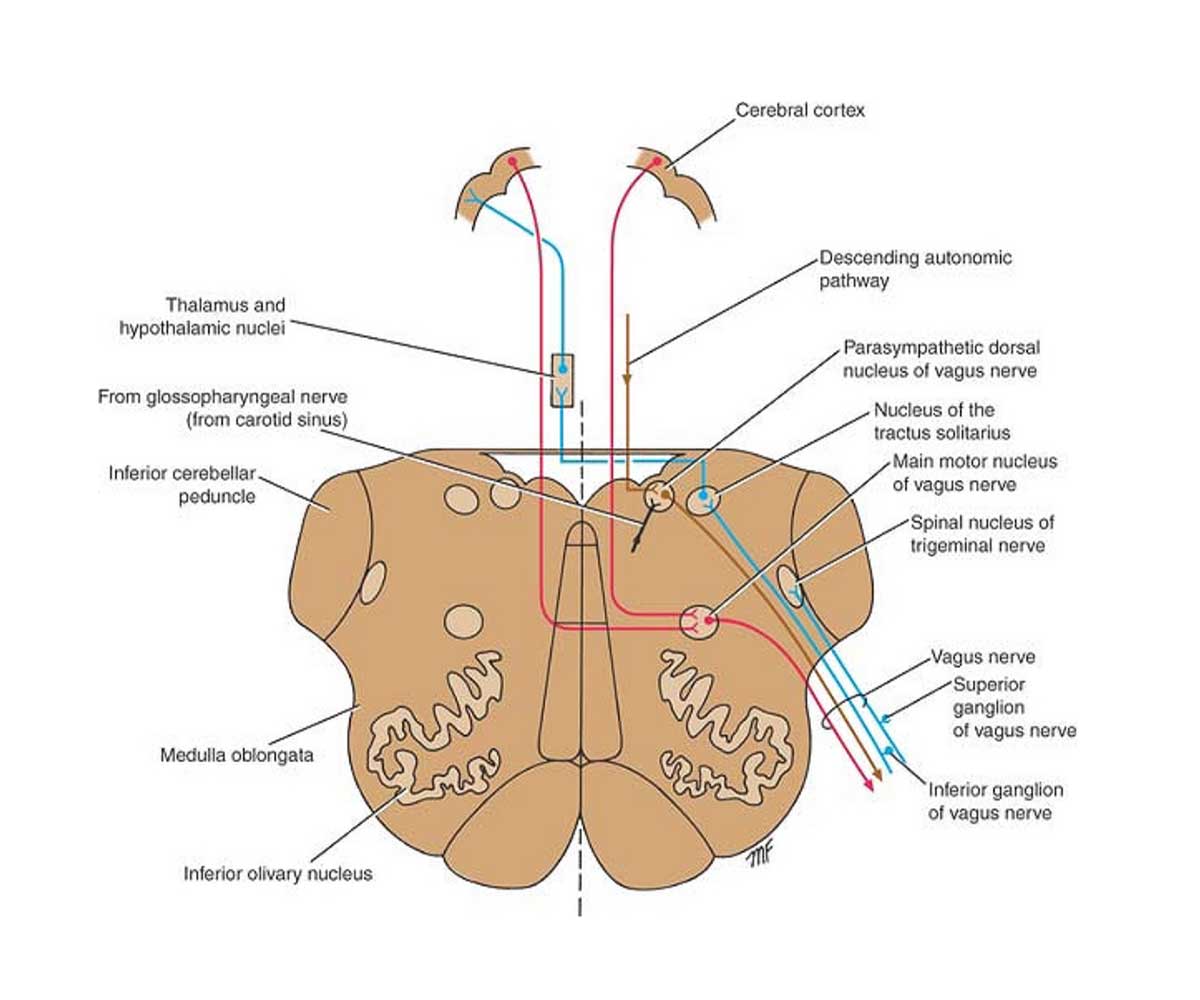
MAIN MOTOR NUCLEUS
The main motor nucleus is one of the 3 major nuclei of the vagus nerve. The integrity of this nucleus is very important for the normal functioning of the vagus nerve. The first thing which is important is to understand the location of the main motor nucleus of the vagus nerve. It lies deep in the reticular formation of the medulla oblongata. Now the function of the reticular formation in this nucleus is to regulate the smooth functioning of neurons in the nucleus. When the vagus nerve is concerned, it helps in performing motor activity.
The cerebrum is divided into two hemispheres and it receives information from the corticonuclear fibers from both the cerebral hemispheres. The corticonuclear tracts provide voluntary control over the muscles of head, neck and face. Therefore the vagus nerve even has a role in it.
In addition to this, the efferents i.e the nerve fibers which take the signal away from the nucleus, go to two places. They supply to the constrictor muscles of the pharynx and the second place to which they supply are the intrinsic muscles of the larynx. Now if something happens to the vagus nerve, the intrinsic muscles of the larynx would not perform their action like production of sounds, closing of and opening of the folds and laryngeal cartilages because the vagus nerve gives rise to recurrent laryngeal nerve which in turn gives rise to inferior laryngeal nerve.
The PARASYMPATHETIC NUCLEUS
It is the second nucleus of the vagus nerve. The parasympathetic nucleus lies in close proximity to the hypoglossal nucleus which is the nucleus of the twelfth cranial nerve. The parasympathetic nucleus forms the dorsal nucleus of the vagus nerve. It lies beneath the floor of the lower part of the fourth ventricle posterolateral to the hypoglossal nucleus. The exact locations of the different anatomical structures define the functional importance of the nerve. Now this parasympathetic nucleus of the vagus nerve receives afferents from different structures. Through the descending autonomic pathways, the nucleus receives afferents, the nerve fibers which are coming from some other structure. It receives afferents from the glossopharyngeal nerve. The major afferents which it receives are from the hypothalamus.
However, the efferent, leave the parasympathetic nucleus and supply different other body parts specifically to the involuntary muscles of bronchi, heart, esophagus, stomach, small intestine, and large intestine only the distal one-third of the transverse colon.
The SENSORY NUCLEUS
The third nucleus of the vagus nerve which is also very important when the sensations conducted by the vagus nerve are concerned is the sensory nucleus.
It is located in the lower part of the nucleus of the tractus solitarius.
Taste sensations are of vital importance. Have you ever noticed that when a person is infected with covid, he or she can not feel the sensation of taste. That is also because the part of this nerve is partially affected which conducts the taste sensations. Sensations of taste travel through the peripheral axons of nerve cells situated in the inferior ganglion on the vagus nerve. That is what the peripheral axons do but the central l processes of those same cells synapse on nerve cells in the nucleus. This completes the connection and helps us to feel the sensations of taste which we do.
Every nucleus sends efferents to different anatomical structures. The efferents from the sensory nucleus cross the median plane and ascend to the ventral group of nuclei of the opposite thalamus. That is if we are discussing the sensory nucleus of the left side, the efferents from its sensory nucleus would go to the thalamus of the opposite i.e right side. Along with the thalamus, they also travel to the hypothalamic nuclei which regulate temperature etc. From the thalamus, the axons of the thalamic cells pass through the internal capsule and corona radiata to end in the postcentral gyrus which lies in the parietal lobe, just posterior to the central sulcus.
Afferent information concerning common sensation enters the brainstem which includes medulla oblongata, pons, diencephalon and midbrain through the superior ganglion of the vagus nerve but ends in the spinal nucleus of the trigeminal nerve.
Hence, all the nerves and their nuclei lie close to each other and work in close proximity.
The Course of Vagus Nerve
Every nerve has its own specific course. Along its course it gives particular branches and eventually exhibits its own function. We will now discuss the course of the vagus nerve. The vagus nerve leaves the anterolateral surface of the upper part of the medulla oblongata as a series of rootlets in a groove between the olive and the inferior cerebellar peduncle of the cerebellum. These rootlets perform their due function in this region. The nerve passes laterally through the posterior cranial fossa which is the area between the jugular foramen and the tentorium cerebelli. Then it leaves the skull through the jugular foramen from where the Cranial nerves IX, X, and XI exit the skull.
Ganglia are clusters of nerve cell bodies found throughout the body. They are part of the peripheral nervous system and carry nerve signals to and from the central nervous system. The vagus nerve possesses two sensory ganglia. The first one is a rounded superior ganglion, situated on the nerve within the jugular foramen. While the second one is cylindrical inferior ganglion, which lies on the nerve just below the foramen. Below the inferior ganglion, the cranial root of the accessory nerve joins the vagus nerve and is distributed mainly in its pharyngeal and recurrent laryngeal branches. Hence the vagus nerve also collaborates with the accessory nerve which is cranial nerve XI for the completion of its function.
After leaving the skull the vagus nerve descends vertically in the neck within the carotid sheath with the internal jugular vein and the internal and common carotid arteries. This carotid sheath is of vital importance. It is present in the neck and its identification carries a lot of importance.
The right hand branch of the vagus nerve
The right vagus nerve enters the thorax and passes posterior to the root of the right lung, contributing to the pulmonary plexus. Hence at first it forms a part of the carotid sheath and now a part of the pulmonary plexus. It then passes on to the posterior surface of the esophagus and contributes to the esophageal plexus. It enters the abdomen through the esophageal opening of the diaphragm. The posterior vagal trunk is distributed to the posterior surface of the stomach and, by a large celiac branch, to the duodenum, liver, kidneys, and small and large intestines as far as the distal third of the transverse colon. This wide distribution is accomplished through the celiac, superior mesenteric, and renal plexuses.
The left-hand branch of the vagus nerve
The left vagus nerve enters the thorax and crosses the left side of the aortic arch and descends behind the root of the left lung, contributing to the pulmonary plexus. The left vagus then descends on the anterior surface of the esophagus, contributing to the esophageal plexus. It enters the abdomen through the esophageal opening of the diaphragm. The anterior vagal trunk divides into several branches, which are distributed to the stomach, liver, upper part of the duodenum, and head of the pancreas.
Therefore, by dividing into left and right branches, the vagus nerve not just supplied to the head and neck region but also supplies to the stomach, small intestine, large intestine, pancreas, lungs, esophagus, pharynx and larynx through different plexuses like esophageal plexus, pulmonary plexus etc.
The image below is a simplified version representing its courses.
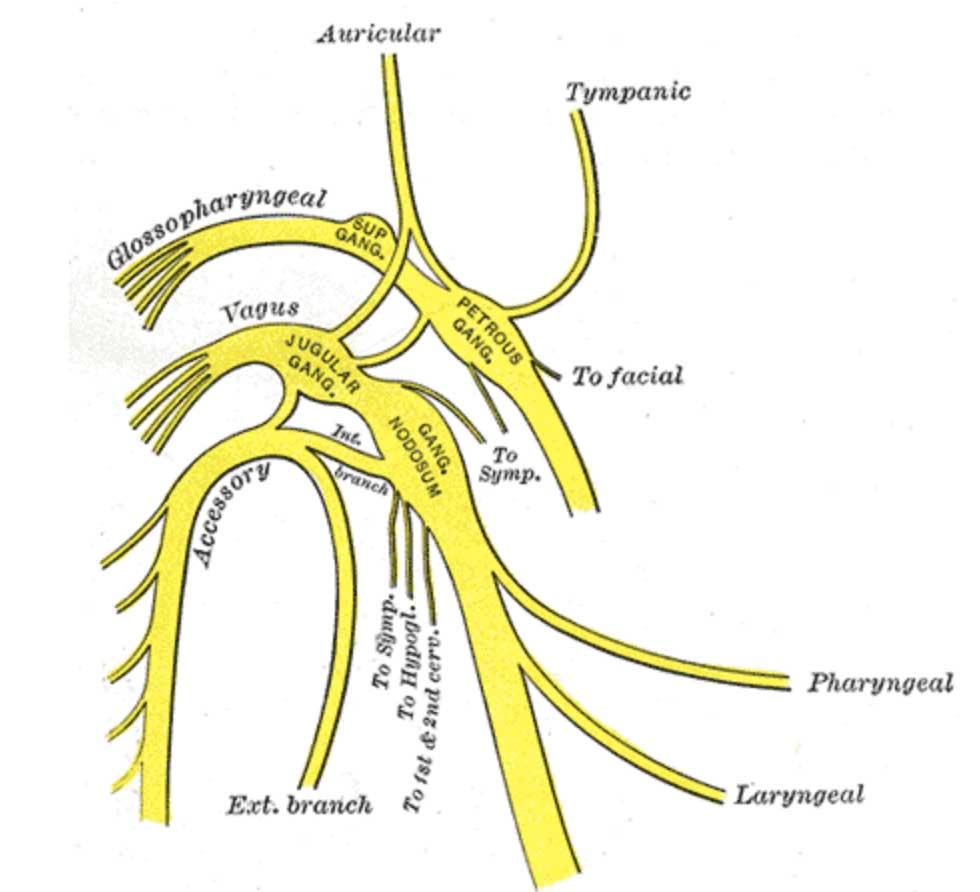
FUNCTIONS OF The VAGUS NERVE
The vagus nerve has various functions. It regulates the internal body functions.
It controls the respiratory rate, the heart rate and the process of digestion. It takes part in all the major activities even the vasomotor functions like coughing, sneezing, vomiting and swallowing.
Whether it is peristalsis or anti-peristalsis, the vagus nerve plays its role. Its anatomical structure is of such an importance that it even supplies to the glands of mucous membrane of the major structures present in the neck for example, pharynx, larynx, organs in the neck, thorax and abdomen.
These are the functions covered by general visceral efferent. In addition to this it also deals with the special visceral efferents, via which it supplies to the skeletal muscles of larynx and pharynx. The heavily supplied pharynx and larynx are working properly partly due to the presence of vagus nerves. It divides and gives branches for their smooth functioning.
It also supplies the ear. The tympanic membrane and external auditory meatus are supplied by the vagus nerve which helps in the functioning of hearing. Other than this, the vagus nerve also provides takes the information and signals from the abdominal viscera like the stomach, pancreas, small and large intestine and from the thoracic viscera like lungs to the valid anatomic structures for proper functioning of abdominal and thoracic viscera. In addition to that, afferents from the aortic arch and body also leave the vagus nerve.
Taste is mainly conducted by various nerves. Vagus nerve also plays its parts when the taste from the epiglottic portion of the tongue is concerned.
CLINICAL TESTING OF VAGUS NERVE TO DETECT ITS FUNCTIONING
We can detect if the vagus nerve is performing its function efficiently or not. For this purpose, different clinical tests are present for example, the palatal arches can be used for this. The size of both the palatal arches are compared.
To analyze if it’s working or not, the uvula is seen. On the paralysed side, there is no arch. However, uvula is pulled to the normal side. Loud gargling with water or loud singing activates our vocal cords which in turn stimulates the vagus nerve. Foot massage which include gentle or firm touch can assist in stimulation the vagus nerve
Different symptoms prove the faulty functioning of the vagus nerve like when the person swallows some liquid it comes out in the form of nasal regurgitation. The liquid starts coming out of the nose. Secondly the voice changes. The voice has a nasal twang to it which is different from the normal sound. At times the voice tends to become hoarse. The palatal arches, when examined, are flattened. Upon different radiological examinations, the vocal cords seem in a cadaveric position which is different from the normal position of the vocal cords. Above all dysphagia is a major symptom. It becomes painfully difficult for the patient to swallow anything. The patient continuously feels that something is stuck in either his throat or chest. Heartburns and regurgitations often accompany it.
In Summary
The vagus nerve is one of the most important cranial nerves in the human body. Which not only transmits all the signals from the body parts like abdominal organs and thoracic organs to the brain and spinal cord, but it also takes efferents from the brain to different organs. The Vagus nerve ensures the smooth functioning of all the body parts. The course of the vagus nerve has been explained in depth above and a simplified version is also demonstrated in an attached picture. It divides into left and right branches and performs its function by giving rootlets everywhere. It even collaborates and mixes with the cranial nerve XI i.e the accessory nerve and supplies accordingly to the sternocleidomastoid and trapezius muscles in the head and neck region.
When this nerve is not functioning properly it presents different signs and symptoms like regurgitation, dysphagia etc so that they can be detected and corrected accordingly. Being the longest cranial nerve in the body which is linked to almost all the systems including the digestive and respiratory systems of the body, it bears a lot of importance.
It contains somatic and visceral afferents along with general and special visceral efferents. Hence, in order to understand the functionality of the vagus nerve we need to understand the anatomy and neuroanatomy of the cerebrum, ganglia, and different nuclei associated with it. Otherwise one can never understand the complexities of the vagus nerve. It is known as the vagus nerve because the word “vagus” literally means a nerve which wanders off to the abdomen.
REFERENCES
⦁ Yuan, H., & Silberstein, S. D. (2016). Vagus Nerve and Vagus Nerve Stimulation, a Comprehensive Review: Part I. Headache, 56(1), 71–78. https://doi.org/10.1111/head.12647
⦁ Farmer, A. D., Albu-Soda, A., & Aziz, Q. (2016). Vagus nerve stimulation in clinical practice. British journal of hospital medicine (London, England : 2005), 77(11), 645–651. https://doi.org/10.12968/hmed.2016.77.11.645
⦁ Yuan, H., & Silberstein, S. D. (2016). Vagus Nerve and Vagus Nerve Stimulation, a Comprehensive Review: Part III. Headache, 56(3), 479–490. https://doi.org/10.1111/head.12649
⦁ Attenello, F., Amar, A. P., Liu, C., & Apuzzo, M. L. (2015). Theoretical Basis of Vagus Nerve Stimulation. Progress in neurological surgery, 29, 20–28. https://doi.org/10.1159/000434652
⦁ Murray, A. R., Atkinson, L., Mahadi, M. K., Deuchars, S. A., & Deuchars, J. (2016). The strange case of the ear and the heart: The auricular vagus nerve and its influence on cardiac control. Autonomic neuroscience : basic & clinical, 199, 48–53. https://doi.org/10.1016/j.autneu.2016.06.004
⦁ HOFFMAN, H. H., & KUNTZ, A. (1957). Vagus nerve components. The Anatomical record, 127(3), 551–567. https://doi.org/10.1002/ar.1091270306
⦁ Hammer, N., Glätzner, J., Feja, C., Kühne, C., Meixensberger, J., Planitzer, U., Schleifenbaum, S., Tillmann, B. N., & Winkler, D. (2015). Human vagus nerve branching in the cervical region. PloS one, 10(2), e0118006. https://doi.org/10.1371/journal.pone.0118006

